As the state moves forward with changes to the Medicaid system through a 1115 Medicaid Waiver, a new and separate Medicaid policy took effect on January 1strelated to co-payments for Medicaid and Medicaid Expansion eligible recipients. Co-payment is an amount of money people pay to a healthcare provider for a health service, such as an office visit or prescription medication. The amount differs depending on the services received and is often paid the day of receiving the service(s). Beginning January 1st, Medicaid recipients, except for children enrolled in Medicaid and KCHIP, children in foster care up to age 26, and pregnant women, are asked to pay a co-payment by their health provider for the services provided.
As the state moves forward with changes to the Medicaid system through a 1115 Medicaid Waiver, a new and separate Medicaid policy took effect on January 1strelated to co-payments for Medicaid and Medicaid Expansion eligible recipients. Co-payment is an amount of money people pay to a healthcare provider for a health service, such as an office visit or prescription medication. The amount differs depending on the services received and is often paid the day of receiving the service(s). Beginning January 1st, Medicaid recipients, except for children enrolled in Medicaid and KCHIP, children in foster care up to age 26, and pregnant women, are asked to pay a co-payment by their health provider for the services provided.
With any change comes questions from effected stakeholders, such as Medicaid-eligible recipients, health providers, and advocates. Below, we have outlined who is affected by this new policy, what services co-payments are applied to, and resources if you have any questions or issues.
Who is impacted by this new policy?
The Cabinet for Health and Family Services exempts children enrolled in Medicaid and KCHIP, children in foster care up to age 26, and pregnant women from this policy change. The policy does note that pregnant women and children can never be refused services for inability to pay. The co-payment policy does apply to parents and other individuals at or below 100% Federal Poverty Line (traditional Medicaid) and they cannot be refused services. Also, the co-payment policy does apply to parents and other individuals between 100% and 138% Federal Poverty Line (Medicaid Expansion). If the parent or individual does not pay the co-payment, the provider has the option to refuse services.
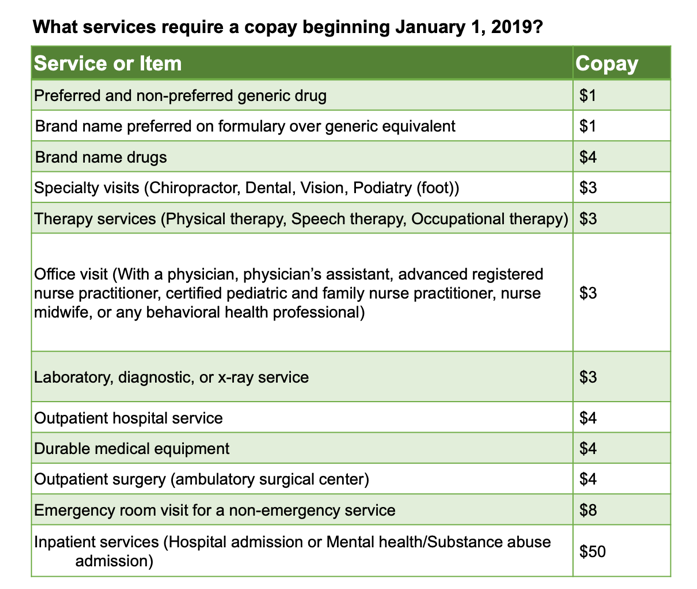
What services require a co-payment?
Preventive services, such as screenings or check-ups, do not have co-payments. Also, emergency services do not have co-payments. Below, you will find a chart with services and the co-payment amount associated with it.
Who can I contact with questions?
Updated resources are available for Medicaid eligible recipients on the Department of Medicaid’s website. For questions and additional resources, please contact your Manage Care Organization (MCO). Phone numbers for each MCO are listed below. If you are Medicaid provider, Department of Medicaid has updated resources available on their provider page.
Manage Care Organizations:
- Aetna: 1-855-300-5528
- Anthem:1-855-690-7784
- Humana Care Source: 1-855-852-7005
- Passport Health Plan:1-800-578-0603
- WellCare: 1-877-389-9457